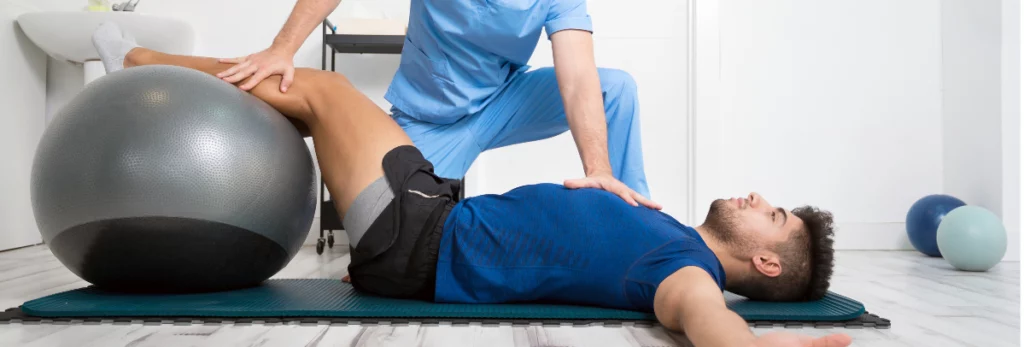
Unlocking the Benefits of Pelvic Floor Physical Therapy
Pelvic floor physical therapy can help strengthen and relax your pelvic floor muscles through targeted exercises and techniques. Read on to learn how this rehabilitation approach may improve bladder control, bowel function, sexual performance, and relieve pain.
Pelvic floor physical therapy (PFPT) is a treatment option that can help individuals experiencing pelvic floor dysfunction. This blog post will explain what pelvic floor physical therapy is, examine its benefits, and provide an overview of what to expect during treatment. With insights from experts and statistics, unlock the full potential of PFPT.
Read time: 9 minutes
What is Pelvic Floor Physical Therapy?
Pelvic floor physical therapy is a type of rehabilitation program that focuses on the muscles, nerves and connective tissues of the pelvic floor region. The pelvic floor is a group of muscles located in the lowest part of the pelvis, supporting the bladder, uterus or prostate, rectum, and vagina in women, and bladder, prostate and rectum in men.
Ready for Relief?
Book Your Next Appointment!According to Dr. D. Lee Bennett, a physical therapist specializing in pelvic health, “Pelvic floor physical therapy is very hands-on, using internal and external soft-tissue and muscular release techniques, biofeedback and effective strengthening programs to return proper function and strength to the pelvic floor.” (Pelvic Rehabilitation Medicine)
Physical therapists who specialize in pelvic floor dysfunction are specially trained to evaluate and treat issues related to pelvic health and pelvic pain. Pelvic floor physical therapists use exercises, manual therapy techniques, biofeedback, and electrical stimulation to help patients strengthen or relax their pelvic floor muscles and address medical conditions like:
- Urinary incontinence or overactive bladder
- Fecal incontinence
- Pelvic organ prolapse
- Painful intercourse
- Chronic pelvic pain
- Constipation
- Other bowel/bladder irregularities
The pelvic floor muscles support the bladder, uterus, and rectum. Weakness or tightness in these muscles can cause issues like incontinence or pain. According to Tara Cortesi, a pelvic floor therapist, “It’s like any other joint in your body. If you break your ankle, you go to physical therapy to work on range of motion, flexibility, and strengthening. The pelvic floor works the same way.” (Herman & Wallace Pelvic Rehabilitation Institute)
Pelvic floor physical therapists receive specialized training to evaluate and treat dysfunction in this sensitive region. The Pelvic Health blog notes these PTs must complete over 100 hours of coursework and demonstrate competency in techniques like manual therapy, biofeedback, and exercise prescription for optimal pelvic floor function. (Resource: WebMD)
Benefits of Pelvic Floor Physical Therapy
Pelvic floor physical therapy offers numerous benefits and can help address a variety of pelvic floor disorders. Here are some of the main advantages:
Improves bladder and bowel control: Physical therapists can help strengthen weakened pelvic floor muscles using Kegel exercises and other techniques. This may reduce urinary or fecal incontinence. According to research by Hirakawa et al. (2013), pelvic floor muscle training significantly decreased urinary incontinence in women at 12 weeks and 1 year after delivery.
Have Questions?
We're Here to Help!Relieves pelvic pain: Pelvic floor PTs perform soft tissue mobilization and trigger point release to reduce muscle spasms, restrictions and pain in the pelvis. One study found that trigger point release and paradoxical relaxation training reduced pelvic pain by an average of 72% (Anderson et al., 2006).
Treats pelvic organ prolapse: Exercises to strengthen the pelvic floor can help support the bladder, uterus and rectum to prevent prolapse. A study by Braekken et al. (2010) found a 29% reduction in pelvic organ prolapse symptoms with pelvic floor muscle training.
Improves sexual performance: For painful intercourse, PTs can help relax tight pelvic floor muscles and increase blood flow. This may improve sexual response and function. One study showed pelvic floor physical therapy decreased dyspareunia by 87% in women with vulvovaginal pain (Goldfinger et al., 2009).
Restores proper alignment and mobility: Therapists correct posture and alignment issues that contribute to pelvic floor dysfunction. PTs also improve coordination of the pelvic floor, abs and back muscles.
Provides postpartum rehab: New moms may experience perineal trauma, weakness or pelvic organ prolapse after childbirth. Pelvic floor therapy can facilitate healing. According to a study by Sampselle et al. (1998), postpartum women doing pelvic floor muscle exercises had significantly improved muscle strength.
Improves quality of life: Pelvic floor disorders can greatly impact daily activities. PFPT aims to help patients regain control and confidence to resume normal activity.
According to research by FitzGerald et al. (2013), 80% of women undergoing pelvic floor physical therapy for urinary incontinence reported significant improvement in their symptoms. And per Rett et al. (2009), pelvic floor rehabilitation led to a 70% average reduction in pelvic pain intensity.
Meet Our Pelvic Floor Specialist
What to Expect During Pelvic Floor Physical Therapy
If you’ve been experiencing pelvic floor dysfunction, urinary/fecal incontinence, or pelvic pain, make an appointment with a pelvic floor physical therapist. Here’s an overview of what to expect:
Initial evaluation: The PT will review your medical history, ask about your symptoms, and perform an external and internal pelvic exam to evaluate the source of dysfunction. They will check for nerve function, muscle tone, pain points, and range of motion.
Looking to Get Started?
Book An Appointment TodayIndividualized treatment plan: The therapist will design a customized treatment plan including exercises and techniques to meet your needs and goals. Treatment plans are tailored to each patient.
Pelvic floor exercises: You’ll learn Kegel exercises and other pelvic stretches and strengthening exercises to perform at home. Proper contracting and relaxing of pelvic floor muscles is key. Pelvic floor exercises may incorporate squats, bridges, breathing techniques, and core engagement.
Manual therapy: Your PT may use massage, trigger point release, or soft tissue mobilization internally or externally to relax tight muscles. According to LaSala et al. (2020), manual therapy can help relax hypertonic PF muscles.
Biofeedback: Sensors provide feedback on how effectively you are contracting the pelvic floor. This helps you gain awareness and control. One study showed that biofeedback training improved stress incontinence (Wang et al., 2011).
Electrical stimulation: Low-voltage electric impulses may help retrain pelvic floor muscle activation. A review by Barroso et al. (2004) found promising evidence for electrical stimulation in treating fecal and urinary incontinence.
Diet/lifestyle recommendations: Your therapist may suggest dietary changes, fluid modifications, exercise tips or posture corrections to facilitate optimal pelvic floor function. Diet and lifestyle adjustments can relieve constipation and pressure on the pelvic floor.
Follow-up visits: You’ll meet regularly with your pelvic floor PT to monitor progress and advance your customized treatment plan. Visits are often weekly at first.
In summary, pelvic floor therapy involves hands-on techniques, personalized exercises and lifestyle adjustments to help strengthen or relax the pelvic floor muscles. Most patients attend sessions 1-2 times per week for 6-12 weeks but treatment plans vary. Don’t hesitate to discuss your symptoms with a doctor to determine if pelvic floor PT may help reduce your discomfort and improve quality of life.
Meet Our Pelvic Floor Specialist
Key Points to Remember
Pelvic floor physical therapy can help treat urinary/fecal incontinence, pelvic organ prolapse, sexual dysfunction and chronic pain through targeted strengthening and relaxation exercises.
Specially trained physical therapists perform internal and external soft tissue techniques and joint mobilization to relieve muscle tension and pain.
Take Control of Your Health
Begin Your Road to RecoveryPatients are prescribed individualized exercise programs to stretch, strengthen and normalize coordination of the pelvic floor muscles.
Up to 80% of patients see significant improvement in symptoms with pelvic floor rehabilitation.
PTs may use biofeedback, electrical stimulation and lifestyle recommendations to facilitate optimal pelvic floor function.
Though effective, pelvic floor therapy requires commitment to regular sessions and daily home exercises. Most patients attend 1-2 times per week for 6-12 weeks.
Don’t suffer in silence with pelvic floor dysfunction. A pelvic health physical therapist can evaluate your symptoms and get you on the path to wellness through customized treatment. Strengthening and relaxing this vital group of muscles may help you regain control and improve quality of life.
Sources
FitzGerald, M. P., Payne, C. K., Lukacz, E. S., Yang, C. C., Peters, K. M., Chai, T. C., . . . Kreder, K. J. (2013). Randomized multicenter clinical trial of myofascial physical therapy in women with interstitial cystitis/painful bladder syndrome and pelvic floor tenderness. Journal of Urology, 189(6), 2113-2118.
Rett, M. T., Simoes, J. A., Herrmann, V., Pinto, C. L., Marques, A. A., & Morais, S. S.
FAQs
Q: What is pelvic floor therapy?
A: Pelvic floor therapy is a specialized form of physical therapy that focuses on treating pelvic floor issues such as pelvic floor dysfunction, pelvic muscle weakness, and pelvic pain. The therapy may include specific exercises to strengthen or relax your pelvic muscles and lifestyle changes to reduce pain.
Q: What are the common causes of pelvic floor dysfunction?
A: Pelvic floor dysfunction can be caused by various factors including chronic constipation, pelvic floor weakness, pregnancy and childbirth, trauma to the pelvic region, and certain medical conditions affecting the pelvic area.
Q: What can I expect during a pelvic floor therapy session?
A: During a pelvic floor therapy session, the therapist will work one-on-one with you to assess your condition, discuss your symptoms and medical history, perform a physical exam of the pelvic region, and develop a personalized treatment plan which may include specific exercises and lifestyle modifications.
Q: How can pelvic floor therapy help with incontinence?
A: Pelvic floor therapy can help with incontinence by teaching you how to properly contract and relax your pelvic floor muscles, improving bladder control and reducing episodes of urgency or leakage.
Q: What are specific exercises involved in pelvic floor therapy?
A: Specific exercises in pelvic floor therapy may include pelvic floor muscle contractions, tailored exercises to strengthen pelvic muscles, and techniques to relax tight pelvic muscles.
Q: What are the qualifications of a pelvic floor therapist?
A: A pelvic floor therapist is a licensed physical therapist with additional specialized training in pelvic health and pelvic floor dysfunction. They are experienced in treating pelvic floor issues and may work with physicians and other healthcare providers to coordinate comprehensive care.
Q: How do I find the right pelvic floor therapist?
A: You can find the right pelvic floor therapist by asking for referrals from your primary care provider, researching therapists experienced in pelvic floor therapy, and ensuring the therapist has the necessary qualifications and experience in treating pelvic floor dysfunction.
Q: Can pelvic floor therapy help with pelvic pain?
A: Yes, pelvic floor therapy can help reduce pelvic pain by addressing muscle tightness, improving pelvic muscle strength and coordination, and promoting perineal healing through specialized techniques and exercises.
Q: What should I expect during a pelvic floor therapy clinic visit?
A: During a visit to a pelvic floor therapy clinic, you can expect a thorough evaluation of your symptoms, a discussion with the therapist about your concerns, and a personalized treatment plan tailored to your specific needs and goals for pelvic health improvement.
Q: Are men and women both eligible for pelvic floor therapy?
A: Yes, both men and women can benefit from pelvic floor therapy. The therapy is designed to address pelvic health issues and pelvic floor dysfunction regardless of gender, and the treatment approach may vary based on individual needs and conditions.

